Abstract
Binge drinking (BD) is an especially pro-oxidant model of alcohol consumption, mainly used by adolescents. It has recently been related to the hepatic IR-process. Skeletal muscle is known to be involved in insulin action and modulation through myokine secretion. However, there is no information on muscle metabolism and myokine secretion after BD exposure in adolescents. Two experimental groups of adolescent rats have been used: control and BD-exposed one. Oxidative balance, energy status and lipid, and protein metabolism have been analyzed in muscle, together with myokine serum levels (IL-6, myostatin, LIF, IL-5, fractalkine, FGF21, irisin, BDNF, FSTL1, apelin, FABP3, osteocrin, osteonectin (SPARC), and oncostatin). In muscle, BD affects the antioxidant enzyme balance leading to lipid and protein oxidation. Besides, it also increases the activation of AMPK and thus contributes to decrease SREBP1 and pmTOR and to increase FOXO3a expressions, promoting lipid and protein degradation. These alterations deeply affect the myokine secretion pattern. This is the first study to examine a general myokine response after exposure to BD. BD not only caused a detrimental imbalance in myokines related to muscle turnover, decreased those contributing to increase IR-process, decreased FST-1 and apelin and their cardioprotective function but also reduced the neuroprotective BDNF. Consequently, BD leads to an important metabolic and energetic disequilibrium in skeletal muscle, which contributes to exacerbate a general IR-process.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Binge drinking (BD) is an acute ethanol (EtOH) consumption model, which brings blood alcohol concentration (BAC) to 0.08 % or higher within 2 h [43]. It has become the most common alcohol consumption pattern used during adolescence [5, 42], a stage especially vulnerable to growth endocrine signals and to the toxic effects of EtOH [2, 41, 45, 47, 48, 64,65,66] predisposing adolescents to future adult metabolic damage [45, 49]. These detrimental effects are due in part to the fact that BD is a particularly pro-oxidant alcohol consumption pattern. It leads to the production of a wide range of reactive oxygen species (ROS) via the microsomal ethanol oxidizing [1, 36]. It also affects the endogenous antioxidant enzyme system in several tissues [47, 48, 64]. This disruption in oxidative balance results in oxidative stress (OS), which compromises, among others, the mitochondrial function, inflammation, and the apoptosis process [47, 48, 64]. OS has also recently been related to a metabolic deregulation process which affects the cellular energy homeostasis mainly in the liver [29]. Specifically, during adolescence, OS generated by BD consumption alters hepatic energy homeostasis through modulating two important regulators of energy metabolism: the NAD+-dependent sirtuin deacetylase (SIRT1) and AMP-activated protein kinase (AMPK) [45]. Both of them restore cellular energy balance by stimulating diverse catabolic processes [7]; therefore, their decrease in liver predisposes to disorders such as insulin resistance (IR) [17, 45, 54]. Lately, IR process is having higher prevalence in adolescents [20] and highly increases the risk of the development of chronic disease over time [55]. For this reason, it is crucial to know what is happening after BD exposure in other insulin responsive tissues, such as skeletal muscle (SKM), which is a primary site for glucose disposal and storage. However, despite chronic-EtOH consumption clinically affects SKM, leading to alcoholic myopathy [53], which it is characterized by muscle atrophy [52], alcohol effects on IR in SKM still remain controversial [28, 30].
When EtOH is consumed acutely during adulthood, it could lead to a breakdown of SKM fibers [62], deeply affecting SKM protein metabolism. It impairs global SKM protein synthesis by a reduction in the mammalian target of rapamycin complex 1 (mTORC1) pathway [32, 69], but it also increases SKM protein degradation by the ubiquitin-proteasome and by the autophagic-lysosomal systems, being this last pathway more profoundly affected [26]. Since muscle proteins not only have a contractile function but they are also a metabolic reserve of amino acids to support tissues’ energetic needs, this catabolic effect clearly has body energy repercussions [26, 68]. The OS and AMPK phosphorylation processes play important roles in protein turnover [22, 31, 63]. It is described that OS mediates EtOH-induced SKM mitochondrial dysfunction and dysregulates not only the protein synthesis and autophagy [31] but also the catabolic ubiquitin-proteasome pathway [27]; these perturbations are reversed by antioxidant treatments. Additionally, in SKM, it has been reported that AMPK activation is directly dependent on the generation of OS, which increases its catabolic actions [70].
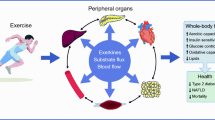
Finally, SKM has been identified as a direct endocrine organ. It releases cytokines and other regulatory peptides which exert paracrine, autocrine, and endocrine effects; they are classified as “myokines” [50]. Recently, novel myokines have been identified, and it has been proved that they may influence metabolism in virtually all organs of the body. Since some of these myokines are induced by SKM contraction and are responsible for mediating energy supply in relation to exercise, they are involved in muscle proliferation. Indeed, they also mediate muscle–organ crosstalk to the brain, adipose tissue, bone, liver, gut, pancreas, vascular bed, and skin in order to balance body energy status [59]. Moreover, their dysregulation is related to metabolic diseases [9, 25] and OS [38]. At the moment, there are just a few studies which analyze several myokines status after chronic alcohol consumption [19], and no data exist after acute one.
The aim of this study is to describe in SKM the effects of BD exposure during adolescence on oxidative and energy balance and their relationship to IR, protein reserves, and myokines secretion.
Materials and methods
Animals
In this experimental protocol, twelve adolescent male Wistar rats (Centre of Production and Animal experimentation, Vice-rector’s Office for Scientific Research, University of Seville) were used. Rats were received at 21 days old and housed in groups of two rats per cage for 1 week in order to acclimatize them to the housing conditions and handling. The experimental treatment was conducted over a 3-week period, beginning when the rats reached postnatal day (PND) 28 and ending at 47 days of age. This period corresponds to adolescence in Wistar rats [16]. The animals were kept at an automatically controlled temperature (22–23 °C) and in a 12-hour light-dark cycle (09:00 to 21:00). Animal care procedures and experimental protocols were performed in accordance with EU regulations (Council Directive 86/609/EEC, November 24th, 1986) and approved by the Ethics Committee of the University of Seville (CEEA-US2019-4).
On PND 28, when the adolescent period began, rats were randomly assigned into two groups (n = 6/group) according to their treatments: control group (C): rats were given control diet and drinking water ad libitum, and on the corresponding days, an isotonic saline solution (SSF) intraperitoneally (i.p.); binge drinking group (BD): rats were given control diet and drinking water ad libitum, and on the corresponding days, an ethanol solution 20% (v/v) in isotonic saline (3 g/Kg/d) i.p. We have previously proven that with this BD experimental model in adolescent Wistar rats BAC was nearly 125.0 mg/dL [44]. In addition, a standard pellet diet (LASQCdiet® Rod14-R, Märkische, Germani) was available ad libitum in all the experimental groups.
Nutritional control
Body weight and the amount of food consumed by rats were monitored daily until the end of the experimental period. The amount of food ingested every day was calculated by measuring this parameter every morning and the next day; the difference between them was the amount consumed. All measurements were taken at 9:00 a.m. to avoid changes due to circadian rhythms.
Ethanol treatment
Alcohol BD-exposed group (BD) received a i.p. injection of alcohol (20 % v/v) in SSF (3 g/Kg/d). Alcohol injections were given starting at 7:00 p.m., when the dark cycle began, for 3 consecutive days each week for 3 weeks. No i.p. injections were given during the remaining 4 days of each week (Nogales et al., 2014). Control group (C) received an i.p. injection of an equal volume of SSF at the same time as the alcohol BD-exposed group’s injections.
Samples
At the end of the experimental period (PND 47), the rats were fasted for 12 h. Then, 24 h after their last EtOH exposure or treatment with saline solution, adolescent rats were anesthetized with an i.p. injection of 28% w/v urethane (0.5 ml/100 g of body weight). The blood was obtained by heart puncture and collected in tubes. The serum was prepared using low-speed centrifugation for 15 min at 1300 × g. Posteriorly, SKM gastrocnemius was removed from the right leg as quickly as possible and immediately frozen in liquid nitrogen and stored at −80 °C. The SKM somatic index (SI) was calculated as SKMSI% = SKM weight/total rat weigh.
Biochemistry parameter analysis
The serum levels of the creatinine and CPK were measured with an automated analyzer (Technicon RA-1000, Bayer Diagnostics, Leverkusen, Germany).
Antioxidant enzymes and oxidative stress markers
In order to measure the activity of antioxidant enzymes (SOD, CAT and GPx) as well as the lipid and protein oxidation, SKM tissue samples were homogenized (100 × g for 1min, 1:4 w/v) using a Potter homogenizer (Pobel 245432, Madrid, Spain) in a sucrose buffer (15 mM Tris/HCl, pH 7.4, 250 mM sucrose, 1 mM EDTA, and 1 mM dithiothreitol) in an ice bath. The homogenate was centrifuged at 900 × g for 10 min at 4 °C. The activity of SOD (U/mg protein) was determined by the Fridovich method, which is based on the ability of SOD to inhibit the reduction of cytochrome c induced by the xanthine-xanthine oxidase system; it is measured by the absorbance increase at 550 nm for 3 min, due to the reduction of cytochrome c by adding xanthine oxidase [15]. Catalase (CAT) activity (U/mg protein) was determined using H2O2 as substrate by the assay of Beers and Sizer [4], where the disappearance of H2O2 was followed spectrophotometrically at 240 nm for 3 min. The GPx activity (mU/mg) was determined using the method described by Lawrence and Burk [33]. In this assay, the oxidized glutathione (GSSG) formed by the action of GPx is coupled to the reaction that catalyzes the glutathione reductase (GR) enzyme, measuring the absorbance decrease at 340 nm for 3 min due to the oxidation of NADPH. In order to measure the OS markers in SKM, the amount of lipid peroxidation was evaluated by the quantification of malondialdehyde (MDA) (mol/mg protein), the end-product of oxidative degradation of lipids, using a colorimetric reaction with thiobarbituric acid (TBA) at 535 nm as described by Draper and Hadley [14]. The protein oxidation was measured by the detection of carbonyl groups (CG) (nmol/mg protein) at 366 nm by the method described by Reznick and Packer [56], where the reaction of 2,4-dinitrophenylhydrazine (DNPH) with CG takes place.
Proteins immunoblotting assays
The expression of the SKM proteins total AMPK (tAMPK), phospho AMPK (pAMPK), SIRT1, IRS-1, mTORC, phospho mTORC (pmTOR), FOXO3a, UKL1, Atrogin-1/MAFBX, and SREBP1 in adolescent rats was conducted using the Laemmli method. The samples utilized contained 60 μg of protein. Proteins were separated on a polyacrylamide gel and were transferred onto a nitrocellulose membrane (BioRad CA, USA) using a blot system (Transblot, BioRad Madrid, Spain). Nonspecific membrane sites were blocked for 1 h with a blocking buffer: TBS (50 mM Tris-HCl1, 150 mM NaCl1, 0.1% (v/v) Tween 20, pH 7.5) and milk powder 3% (BioRad Madrid, Spain), and thereafter, they were probed overnight at 4 °C with the following specific primary antibodies: SIRT1, pAMPKα, and IRS-1 (Cell Signaling Techonology); and tAMPKα, SREBP1, mTOR, pmTOR, FOXO3a, UKL1, and Atrogin-1/MAFBX (Santa Cruz Biotechnology Heidelberg, Germany). Then, membranes were incubated with secondary antibodies (antirabbit or antimouse IgG HRP conjugate, BioRad, Madrid, Spain). Monoclonal mouse anti-GAPDH (Santa Cruz Biotechnology) was used as a loading control, followed by the secondary antibody antimouse IgG Peroxidase conjugate (A9044, Sigma-Aldrich, Spain). The membranes were incubated for 1 min with the commercial developer solution Luminol ECL reagent (GE Healthcare and Lumigen, Buckinghamshire, UK) and analyzed with the Amersham Imager 600 (GE Healthcare, Buckinghamshire, UK). Then, the quantification of the blots was performed by densitometry with the ImageJ program. The results were expressed as percent arbitrary relative units, referring to values in control animals which were defined as 100%.
Myokines determination
Serum myokine levels, such as IL-6, myostatin, LIF, IL-5, fraktalkine (CX3CL1), FGF21, irisin, BDNF, FSTL1, apelin, FABP3, osteocrin, osteonectin (SPARC), and oncostatin, were measured using MILLIPLEX® Rat Myokine Panel (Millipore Corp., St. Charles, MO, USA), based on immunoassays on the surface of fluorescent-coded beads (microspheres), following the specifications of the manufacturer (50 events per bead, 50 μL sample, gate settings of 8000–15000, time out of 60 s, melatonin bead set of 34). The plate was read on a LABScan 100 analyzer (Luminex Corp., Austin, TX, USA) with xPONENT software for data acquisition. Average values for each set of duplicate samples or standards were within 15% of the mean. Myokines concentrations in plasma samples were determined by comparing the mean of duplicate samples with the standard curve for each assay.
Statistical analysis
The results are expressed as means ± standard error of the mean (SEM). The data were analyzed using a statistical program Statistica Version 12.0 (StatSoft, Tulsa, OK, USA). To assess difference between C and BD groups, the non-parametric Mann–Whitney–Wilcoxon test was used. The statistical significance was established at p < 0.05.
Results
The results showed that BD exposure during adolescence leads to a lower body weight (p < 0.05), without significantly affecting SKM mass (Table 1). Regarding SKM, protein concentration, serum creatinine, and CPK levels remained all of them invariable.
Figure 1 shows that adolescent rats exposed to BD present a significant increase in SOD and CAT activities (p < 0.01 and p < 0.05, respectively) and a decrease in GPx activity (p < 0.05), which lead to an oxidative lipid and protein profile (p <0.01).
Skeletal muscle oxidative balance after BD exposure. A Superoxide dismutase (SOD). B Catalase (CAT). C Glutathione peroxidase (GPx) enzymes. D Oxidation of protein (carbonil group (CG) levels). E Lipid peroxidation (malondialdehyde (MDA) levels). The results are expressed as mean ± SEM and analyzed by nonparametric Mann–Whitney–Wilcoxon test. The number of animals in each group is six. Groups: C: control group, BD: binge drinking group. Statistic difference between groups was expressed as p value: C vs BD: *p < 0.05, **p < 0.01
Respect to energy marker proteins (Fig. 2), BD exposure does not affect SIRT1 expression and decreases tAMPKα expression (p < 0.01). However, alcohol consumption activates AMPK function since it increases pAMPKα expression and thus pAMPK/tAMPK ratio (p < 0.01). This increase is in concordance with the lower SREBP1 expression values found after BD exposure (p < 0.01). Furthermore, protein turnover is significantly affected by BD (p < 0.05), since pmTOR expression decreased whereas FOXO3a expression increased (p < 0.05) (Fig. 3). In this context, Atrogin-1/MAFBX and ULK1, both involved in protein degradation, were increased (p < 0.05).
Expression of main energetic regulators in skeletal muscle. A SIRT1. B tAMPK. C pAMPK. D AMPK activation ratio. E Expression lipogenic transcription factor SREBP. F Representative western blots of proteins (normalized to GAPDH). The results are expressed as mean ± SEM and analyzed nonparametric Mann–Whitney–Wilcoxon test. The number of animals in each group is six. Groups: C: control group, BD: binge drinking group. Statistic difference between groups was expressed as p value: **p < 0.01
Expression of main transcription factors implicated in protein metabolism of skeletal muscle: A mTOR. B pmTOR. C FOXO3a. D ULK1. E Atrogin-1/MAFBX. F Representative western blots of proteins (normalized to GAPDH). The results are expressed as mean ± SEM and analyzed by nonparametric Mann–Whitney–Wilcoxon test. The number of animals in each group is six. Groups: C: control group, BD: binge drinking group. Statistic difference between groups was expressed as p value: *p < 0.05
In adolescent rats, glucose serum levels were significantly increased after BD exposure (p < 0.05) (Fig. 4); however, IRS-1 expression in SKM decreased (p < 0.05). To conclude, BD exposure during adolescence significantly alters myokines serum values (Table 2). BD not only increases IL-6 and myostatin (p < 0.05) serum levels but it also decreases LIF (p < 0.05), CX3CL1 (p < 0.01), FGF21 (p < 0.01), irisin (p < 0.01), BDNF (p < 0.01), FSTL-1 (p < 0.01), apelin (p < 0.01), and SPARC (p < 0.05) values.
Serum glucose concentration (A) and expression of IRS1 in skeletal muscle (B). C Representative western blots of IRS1 (normalized to GAPDH). The results are expressed as mean ± SEM and analyzed by nonparametric Mann–Whitney–Wilcoxon test. The number of animals in each group is six. Groups: C: control group, BD: binge drinking group. Statistic difference between groups was expressed as p value: *p < 0.05
Discussion
BD exposure does not impact the overall morphological characteristics of skeletal muscle
Despite the fact that EtOH consumption does not change the amount of food intake, BD rats presented a lower increase in body weight, without affecting their length, probably related to a lower adipose mass. However, general parameters relative to SKM anabolism and catabolism processes such as SKMSI, protein muscle content, serum creatinine, and CPK values remained significantly unaffected. Since proteins are the best conserved macromolecules in the body, these effects could be postponed in time. Nevertheless, a tendency to a decrease in SKM protein content seems to be occurring.
BD exposure leads to oxidative damage in skeletal muscle and to an increase in AMPKα activation, avoiding lipogenesis
BD exposure during adolescence changes the antioxidant balance activity in the gastrocnemius muscle (Fig. 5). It leads to an increased activity of SOD and CAT; however, these higher activities generated due to EtOH exposure to combat ROS were not efficient, since lipid and protein oxidation appeared in any case. Therefore, like in serum, liver, kidney, and heart [46,47,48,49, 64], BD exposure during adolescence is also a potent pro-oxidant in the gastrocnemius muscle.
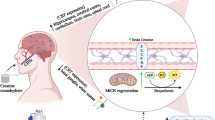
Effect of BD exposure during adolescence on skeletal muscle metabolism and myokine secretion. When EtOH is consumed in large amounts, as in BD exposure, it arrives at other tissues like SKM. This EtOH generates a great amount of reactive oxygen species, which in the end lead to the appearance of oxidative stress. Consequently, the expression ratio of pAMPK/tAMPK increases, resulting in a stimulated AMPK function. The active AMPK, as an important energy status sensor, regulates several other proteins. On the one hand, it inhibits the expression of SREBP1 and mTOR, which, respectively, will decrease the lipid and protein synthesis; on the other hand, AMPK stimulates FOXO3a and ULK1 expressions. FOXO3a will result in the stimulation of the protein breakdown pathways: it promotes the initiation of autophagy; and increasing the Atrogin-1/MAFBX expression, it also activates the proteosome system. Besides, ULK1, together with FOXO3a, will stimulate the initiation of autophagy and the mitochondrial autophagy process (mitophagy). Additionally, the oxidative stress diminishes the expression of IRS-1, which will not stimulate Akt. This protein, when active, stimulates mTOR and inhibits FOXO3a; in this case, being inactive, it will produce the opposite effects, promoting a general IR process. Furthermore, EtOH exposition seriously affects myokine secretion to serum, increasing IL-6 and myostatin levels and decreasing BDNF, fractalkine, FGF21, irisin, LIF, and SPARC values. This altered pattern of secretion contributes to the muscular destruction, the insulin resistance, and to the development of a cognitive impairment. In summary, BD exposition promoted the lipolysis and protein degradation in SKM and inhibited protein synthesis and lipogenesis, also altering the insulin signaling pathway, contributing to a general IR process. Solid lines and hatched lines indicate stimulatory and inhibitory actions, respectively
OS is deeply related to the energetic cellular balance. BD-OS generated in liver contributes to a decrease in SIRT1 and AMPK activation [45]. However, in SKM, despite the fact that OS appears, SIRT1 expression remains unaffected, and AMPKα activation is enhanced. Previous studies describe that in SKM, AMPK is clearly activated by OS, independently of changes in the AMP/ATP ratio [70].
Moreover, it has been determined in myotubes that an increase in the myokine IL-6 activates AMPKα subunit [8]. In this study, IL-6 serum levels are markedly increased after BD exposure and could be contributing to the AMPK activation. Indeed, several authors have described the effects of IL-6 in SKM fatty acid metabolism in human and in vitro, confirming that it activates lipolysis independently of hormonal signals, increasing rates of fatty acid oxidation and pointing to AMPKα as a possible master key [6].
SREBP1 is a key lipogenic transcription factor which is up-regulated by glucose and insulin and down-regulated by AMPK in SKM, pointing to AMPKα as an effective approach to avoid tissue lipogenesis [23]. In the present study, the higher pAMPK expression found in BD rats is in concordance with the lower SREBP1 values found, indicating that lipolysis is taking place in SKM. This fact coupled with lipid oxidation indicates that lipid homeostasis is definitely damaged in this tissue.
BD exposure affects protein turnover homeostasis by enhancing oxidative stress and the AMPKα-FOXO3a axis
There are different signaling pathways which connect OS to decreased protein synthesis and increased proteolysis patterns. OS contributes to SKM protein catabolism by increasing the expression of proteins involved in autophagy and the proteasome system of proteolysis; it also activates muscle proteases such as caspases and calpains; and it affects the structure of myofibrillar proteins favoring proteolytic processes. Moreover, it also contributes to depress global SKM protein synthesis by affecting mTOR signaling; however, most of these studies are still in vitro [18, 51]. Finally, OS in SKM leads to AMPKα activation [70].
AMPKα activity in SKM is known to govern protein turnover mainly towards a catabolic state by directly increasing the mammalian autophagy-initiating kinase ULK1 and the transcription factor FOXO3a activities, both related to protein breakdown; but it also acts by decreasing mTOR activity, which is related to protein synthesis [58]. AMPKα also promotes mitochondrial biogenesis to produce more ATP. The AMPKα-ULK1 axis is deeply related not only to autophagy initiation but also to the mitochondrial autophagy (mitophagy) process [21]. The AMPK-FOXO3a axis is a potent myofibrillar proteolytic system that activates the ubiquitin-proteosome system by increasing a muscle specific F-box protein, Atrogin-1, also known as MAFBX, which is a principal component of the SCF ubiquitin ligase complex that ubiquitinates and targets calcineurin for degradation. FOXO3a also activates the autophagosome-lysosome system and the mitophagy process [57]. As a consequence, the higher OS and the pAMPKα levels found in BD rats result in higher FOXO3a, Atrogin-1, and ULK1 levels, and lower pmTORC1 expressions [24]. These results clearly imply that lower protein synthesis and higher protein destruction have taken place after BD exposure. Together with the high protein oxidation found, it is clear that BD exposure during adolescence affects protein metabolism and function in the SKM.
BD exposure seems to promote insulin resistance in SKM
Therefore, SKM dysfunction during BD exposure contributes to a disruption in lipid and protein homeostasis; moreover, it seems to promote the instauration of the insulin resistance process, since in SKM IRS-1 expression is decreased and hyperglycemia is appearing [16]. It is described that OS in mammalian SKM in vitro cells leads to a loss of IRS-1 protein, in part due to a p38 MAPK-dependent mechanism [3]. Therefore, the OS detected in this study could be contributing to induce IR. The anabolic insulin signaling process activates the phosphoinositide 3-kinase (PI3K)/Akt pathway. Akt not only phosphorylates many proteins such as mTOR and SREBP1, resulting in augmented protein and lipid synthesis [12], but it also has a downstream effect on FOXO3a, avoiding protein degradation [37]. According to that, after BD exposure, pmTORC1 and SREBP1 expressions are decreased, and FOXO3a expression is enhanced, indicating that the insulin-Akt axis is not effectively acting in SKM, which is consistent to an IR instauration.
BD exposure clearly modulates the myokine secretion pattern associated with insulin resistance
The SKM not only excretes myokines in order to maintain its own homeostasis but it also has a direct influence on the general energy status. Like in hepatic steatosis, where there is an imbalance in myokine, hepatokine, and adipokine secretions, which are implicated in negative metabolic processes [13], in BD-exposed adolescent rats, which present hepatic alcoholic damage [45], it may also happen. Consequently, it is important to know the myokines balance after BD exposure. In this study, for the first time, it is demonstrated that EtOH exposure seriously affects myokine secretion, having important metabolic and energetic repercussions even during adolescence.
In this context, BD exposure during adolescence increased IL-6 and myostatin serum levels, two myokines that increase muscle atrophy, decrease muscle mass, and lead to fatty acid oxidation in muscle by different mechanisms [35, 38]. They are presumably contributing to the occurrence of biomolecular changes in the SKM protein synthesis route described above after BD exposure, promoting protein catabolism. Nevertheless, in order to have macroscopic repercussions, a longer EtOH exposure would probably be needed. Besides, it is also described that myostatin increases ROS generation in SKM through the NF-κB pathway, which is also related to inflammation [67]. Therefore, myostatin could be another pro-oxidant factor in the OS generated in SKM after BD exposure. IL-6 signaling has also been associated with stimulation of lipolysis and adipose browning by the activation of AMPK [71]. In addition, IL-6 mediates a cross-talk between insulin-sensitive tissues, among others by increasing glucose release by liver [13, 59]. The elevated IL-6 values found after BD confirm the hyperglycemia and the lower IRS-1 expression detected, being this myokine contributing to the general BD-IR process.
In contrast, BD exposure decreased SPARC, LIF, CX3CL1, FGF21, irisin, and BDNF serum levels. All of them have anabolic effects on SKM such as the stimulation of the proliferation of myoblast, an increased muscle mass and muscle regeneration, or an increased mitochondria biogenesis, to name but a few [35]. These proteins’ decreases contribute to the SKM catabolic state generated by BD exposure, and difficult SKM remodeling. Moreover, CX3CL1, FGF21, and irisin promote glucose uptake, protect beta-cell from inflammation, increase insulin sensitivity in muscle, and lead to adipose browning; all these effects decrease the IR process [13, 59, 60]. Since they are decreased, IR process is probably taking place, at least in part by the damage generated by BD to SKM. Furthermore, BDNF is involved in neurogenesis and in the protection against oxidative damage and neuronal apoptosis. Its increase promotes synaptic plasticity in hippocampal neurons, neurogenesis, and memory and learning processes [39]. Therefore, the reduced BDNF found in these BD rats may also be associated with the well-known neurotoxic effects of EtOH consumption during adolescence, being many of these effects specific to adolescents and not found in parallel adult studies [10].
Additionally, BD exposure also decreases serum levels of the myokines FST-1 and apelin; both of them are related to the endothelial function, revascularization, cardioprotection, and blood pressure regulation [9, 13, 59, 60]. These results are in agreement with those obtained in a similar BD experimental model by Ojeda et al. [48], where BD exposure led to OS, inflammation, and apoptosis in cardiac myocytes and to an increase in the endothelial markers CTGF, VEGF, tPAI-1, and cav-1, joint to a higher blood pressure and heart rate. These results point to SKM as a master key not only in metabolic and energy balance but also in cardiovascular modulation after BD exposure.
FGF21 and FSTL-1 serum levels are significantly the most affected myokines by BD exposure. Both of them have the liver as a cross-talk organ [9] and are also secreted by liver [13], being considered hepatokines. They have beneficial actions on the hepatic metabolism. Among other functions, FGF21 increases the oxidation of fatty acids in the liver, reverses hepatic steatosis, and increases energy expenditure [13, 34, 40]; in BD-exposed adolescent rats, its reduction is in concordance with the liver steatosis found. FSTL-1 plays a crucial role in liver fibrosis [61], being its decrease related to the liver damage caused by the acute EtOH ingestion [11, 45, 47].
Finally, according to the rats’ final body length, BD exposure has no repercussion on those myokines related to bone remodeling and function, such as osteocrin and oncostatin. As for IL-15 and FABP3 serum levels, they were also unaffected by BD exposure.
Consequently, it has been demonstrated that BD exposure during adolescence clearly disrupts the SKM through the OS generated, affecting the metabolic and energy balance, and the SKM structure and function. These imbalances have deep important endocrine repercussions. In summary, for the first time, it has been demonstrated that BD-SKM damage has general endocrine repercussions via myokines, especially by those related to muscle protein loss, the IR process and glucose uptake, lipolysis, and the adipose browning, affecting the metabolic and energetic body balance and the hepatic health. Furthermore, since BDNF serum levels are reduced, it could be promoting EtOH neurotoxic effects. All in all, these findings support the hypothesis that adolescent BD promotes SKM atrophy, which could lead to long-lasting changes in the adult metabolism, increasing risks for future cardiopathologies.
References
Abdelmegeed MA, Banerjee A, Jang S, Yoo SH, Yun JW, Gonzalez FJ, Keshavarzian A, Song BJ (2013) CYP2E1 potentiates binge alcohol-induced gut leakiness, steatohepatitis, and apoptosis. Free Radic Biol Med 65:1238–1245
Ai L, Perez E, Asimes A, Kampaengsri T, Heroux M, Zlobin A, Hiske MA, Chung CS, Pak TR, Kirk JA (2020) Binge alcohol exposure in adolescence impairs normal heart growth. J Am Heart Assoc 9:15611
Archuleta TL, Lemieux AM, Saengsirisuwan V, Teachey MK, Lindborg KA, Kim JS, Henriksen EJ (2009) Oxidant stress-induced loss of IRS-1 and IRS-2 proteins in rat skeletal muscle: role of p38 MAPK. Free Radic Biol Med 47:1486–1493
Beers RF, Sizer IW (1952) A spectrophotometric method for measuring the breakdown of hydrogen peroxide by catalase. J Biol Chem 195:133–140
Bonar EE, Parks MJ, Gunlicks-Stoessel M, Lyden GR, Mehus CJ, Morrell N, Patrick ME (2021) Binge drinking before and after a COVID-19 campus closure among first-year college students. Addict Behav 118:106879
Bruce CR, Dyck DJ (2004) Cytokine regulation of skeletal muscle fatty acid metabolism: effect of interleukin-6 and tumor necrosis factor-alpha. Am J Physiol Endocrinol Metab 287
Cantó C, Auwerx J (2009) PGC-1α, SIRT1 and AMPK, an energy sensing network that controls energy expenditure. Curr Opin Lipidol 20:98–105
Carey AL, Steinberg GR, Macaulay SL, Thomas WG, Holmes AG, Ramm G, Prelovsek O, Hohnen-Behrens C, Watt MJ, James DE, Kemp BE, Pedersen BK, Febbraio MA (2006) Interleukin-6 increases insulin-stimulated glucose disposal in humans and glucose uptake and fatty acid oxidation in vitro via AMP-activated protein kinase. Diabetes 55:2688–2697
Chen W, Wang L, You W, Shan T (2021) Myokines mediate the cross talk between skeletal muscle and other organs. J Cell Physiol 236:2393–2412
Crews FT, Vetreno RP, Broadwater MA, Robinson DL (2016) Adolescent alcohol exposure persistently impacts adult neurobiology and behavior. Pharmacol Rev 68:1074–1109
del C. Gallego-Lopez M, Ojeda ML, Romero-Herrera I, Nogales F, Carreras O (2022) Folic acid homeostasis and its pathways related to hepatic oxidation in adolescent rats exposed to binge drinking. Antioxidants 11(2022):362.11–362.362362
Dibble CC, Cantley LC (2015) Regulation of mTORC1 by PI3K signaling. Trends Cell Biol 25:545–555
Dos Santos AR de O, de Zanuso BO, Miola VFB, Barbalho SM, Santos Bueno PC, Flato UAP, Detregiachi CRP, Buchaim DV, Buchaim RL, Tofano RJ, Mendes CG, Tofano VAC, Dos Santos JF (2021) Haber Adipokines, myokines, and hepatokines: crosstalk and metabolic repercussions. Int J Mol Sci 22:1–23
Draper HH, Hadley M (1990) Malondialdehyde determination as index of lipid Peroxidation. Methods Enzymol 186:421–431
Fridovich I (1985) Cytochrome c, in: R.A. Greenwald (Ed.), CRC Handb. Methods Oxyg. Radic. Res., 1st Edition, CRC Press: pp. 213–216
Furukawa S, Fujita T, Shimabukuro M, Iwaki M, Yamada Y, Nakajima Y, Nakayama O, Makishima M, Matsuda M, Shimomura I (2017) Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Invest 114:1752–1761
Giovannini L, Bianchi S (2017) Role of nutraceutical SIRT1 modulators in AMPK and mTOR pathway: evidence of a synergistic effect. Nutrition 34:82–96
Gonzalez A, Simon F, Achiardi O, Vilos C, Cabrera D, Cabello-Verrugio C (2021) The critical role of oxidative stress in sarcopenic obesity. Oxid Med Cell Longev 2021
González-Reimers E, Fernández-Rodríguez CM, Santolaria-Fernández F, de la Vega-Prieto MJ, Martín-González C, Gómez-Rodríguez MA, Alemán-Valls MR, Rodríguez-Gaspar M (2011) Interleukin-15 and other myokines in chronic alcoholics. Alcohol Alcohol 46:529–533
Higgins V, Adeli K (2017) Pediatric metabolic syndrome: pathophysiology and laboratory assessment. EJIFCC 28:25–42
Iorio R, Celenza G, Petricca S (2021) Mitophagy: molecular mechanisms, new concepts on parkin activation and the emerging role of AMPK/ULK1 axis, Cells 11
Ismaeel A, Laudato JA, Fletcher E, Papoutsi E, Tice A, Hwa LS, Miserlis D, Jamurtas AZ, Steiner J, Koutakis P (2022) High-fat diet augments the effect of alcohol on skeletal muscle mitochondrial dysfunction in mice, Nutrients 14
Jayachandran M, Zhang T, Wu Z, Liu Y, Xu B (2020) Isoquercetin regulates SREBP-1C via AMPK pathway in skeletal muscle to exert antihyperlipidemic and anti-inflammatory effects in STZ induced diabetic rats. Mol Biol Rep 47:593–602
Kahn BB, Alquier T, Carling D, Hardie DG (2005) AMP-activated protein kinase: ancient energy gauge provides clues to modern understanding of metabolism. Cell Metab 1:15–25
Karstoft K, Pedersen BK (2016) Skeletal muscle as a gene regulatory endocrine organ. Curr Opin Clin Nutr Metab Care 19:270–275
Kimball SR, Lang CH (2018) Mechanisms underlying muscle protein imbalance induced by alcohol. Annu Rev Nutr 38:197–217
Kobayashi H, Nakamura S, Sato Y, Kobayashi T, Miyamoto K, Oya A, Matsumoto M, Nakamura M, Kanaji A, Miyamoto T (2021) ALDH2 mutation promotes skeletal muscle atrophy in mice via accumulation of oxidative stress, Bone 142
Koh JH, Kim KH, Park SY, Kim YW, Kim JY (2020) PPARδ attenuates alcohol-mediated insulin resistance by enhancing fatty acid-induced mitochondrial uncoupling and antioxidant defense in skeletal muscle, Front Physiol 11
Kołota A, Głąbska D, Oczkowski M, Gromadzka-Ostrowska J (2020) Oxidative stress parameters in the liver of growing male rats receiving various alcoholic beverages. Nutr 12:158.12–158.158158
Kumar V, Frost RA, Lang CH (2002) Alcohol impairs insulin and IGF-I stimulation of S6K1 but not 4E-BP1 in skeletal muscle. Am J Physiol Endocrinol Metab 283
Kumar A, Davuluri G, Welch N, Kim A, Gangadhariah M, Allawy A, Priyadarshini A, McMullen MR, Sandlers Y, Willard B, Hoppel CL, Nagy LE, Dasarathy S (2019) Oxidative stress mediates ethanol-induced skeletal muscle mitochondrial dysfunction and dysregulated protein synthesis and autophagy. Free Radic Biol Med 145:284–299
Laufenberg LJ, Crowell KT, Lang CH (2021) Alcohol acutely antagonizes refeeding-induced alterations in the Rag GTPase-Ragulator complex in skeletal muscle. Nutrients 13
Lawrence RA, Burk RF (1976) Glutathione peroxidase activity in selenium-deficient rat liver. Biochem Biophys Res Commun 71:952–958
Lebensztejn DM, Flisiak-Jackiewicz M, Białokoz-Kalinowska I, Bobrus-Chociej A, Kowalska I (2016) Hepatokines and non-alcoholic fatty liver disease. Acta Biochim Pol 63:459–467
Lee JH, Jun HS (2019) Role of myokines in regulating skeletal muscle mass and function. Front Physiol 10:42
Lu Y, Cederbaum AI (2008) CYP2E1 and oxidative liver injury by alcohol. Free Radic Biol Med 44:723–738
Mammucari C, Schiaffino S, Sandri M (2008) Downstream of Akt: FoxO3 and mTOR in the regulation of autophagy in skeletal muscle. Autophagy 4:524–526
Mancinelli R, Checcaglini F, Coscia F, Gigliotti P, Fulle S, Fanò-Illic G (2021) Biological aspects of selected myokines in skeletal muscle: focus on aging. Int J Mol Sci 22
Martín-González C, Romero-Acevedo L, Fernández-Rodríguez CM, Medina-Vega L, García-Rodríguez A, Ortega-Toledo P, González-Navarrete L, Vera-Delgado VE, González-Reimers E (2021) Brain-derived neurotrophic factor among patients with alcoholism. CNS Spectr 26:400–405
Meex RCR, Watt MJ (2017) Hepatokines: linking nonalcoholic fatty liver disease and insulin resistance. Nat Rev Endocrinol 139(13):509–520
Molina PE, Nelson S (2018) Binge drinking’s effects on the body. Alcohol Res 39:99–109
Muzi S, Sansò A, Pace CS (2021) What’s happened to Italian adolescents during the COVID-19 pandemic? A preliminary study on symptoms, problematic social media usage, and attachment: relationships and differences with pre-pandemic peers. Front Psychiat 12:590543
National Institute on Alcohol Abuse and Alcoholism (2020) What is binge drinking?
Nogales F, Rua RM, Ojeda ML, Murillo ML, Carreras O (2014) Oral or intraperitoneal binge drinking and oxidative balance in adolescent rats. Chem Res Toxicol 27
Nogales F, Cebadero O, Romero-Herrera I, Rua RM, Carreras O, Ojeda ML (2021) Selenite supplementation modulates the hepatic metabolic sensors AMPK and SIRT1 in binge drinking exposed adolescent rats by avoiding oxidative stress. Food Funct 12:3022–3032
Ojeda ML, Rua RM, Nogales F, Díaz-Castro J, Murillo ML, Carreras O (2016) The benefits of administering folic acid in order to combat the oxidative damage caused by binge drinking in adolescent rats. Alcohol Alcohol 51:235–241
Ojeda ML, Carreras O, Sobrino P, Murillo ML, Nogales F (2017) Biological implications of selenium in adolescent rats exposed to binge drinking: oxidative, immunologic and apoptotic balance. Toxicol Appl Pharmacol 329
Ojeda ML, Sobrino P, Rua RM, Gallego-Lopez MC, Nogales F, Carreras O (2021) Selenium, a dietary-antioxidant with cardioprotective effects, prevents the impairments in heart rate and systolic blood pressure in adolescent rats exposed to binge drinking. Am J Drug Alcohol Abuse
Ojeda ML, Nogales F, del Carmen Gallego-López M, Carreras O (2022) Binge drinking during the adolescence period causes oxidative damage-induced cardiometabolic disorders: a possible ameliorative approach with selenium supplementation. Life Sci. 301:120618
Pedersen BK, Febbraio MA (2008) Muscle as an endocrine organ: focus on muscle-derived interleukin-6. Physiol Rev 88:1379–1406
Powers SK, Smuder AJ, Criswell DS (2011) Mechanistic links between oxidative stress and disuse muscle atrophy. Antioxid Redox Signal 15:2519–2528
Preedy VR, Peters TJ (1990) Alcohol and skeletal muscle disease. Alcohol Alcohol 25:177–187
Preedy VR, Paice A, Mantle D, Dhillon AS, Palmer TN, Peters TJ (2001) Alcoholic myopathy: biochemical mechanisms. Drug Alcohol Depend 63:199–205
Reaven GM (1995) Pathophysiology of insulin resistance in human disease. Physiol Rev 75:473–486
Reaven G (2012) Insulin resistance and coronary heart disease in nondiabetic individuals. Arterioscler Thromb Vasc Biol 32:1754–1759
Reznick AZ, Packer L (1994) [38] Oxidative damage to proteins: spectrophotometric method for carbonyl assay. Methods Enzymol 233:357–363
Sanchez AMJ, Candau RB, Bernardi H (2014) FoxO transcription factors: their roles in the maintenance of skeletal muscle homeostasis. Cell Mol Life Sci 71:1657–1671
Sanchez A, Candau R, Bernardi H (2019) Recent data on cellular component turnover: focus on adaptations to physical exercise. Cells 8:542
Severinsen MCK, Pedersen BK (2020) Muscle-organ crosstalk: the emerging roles of myokines. Endocr Rev 41:594–609
Severinsen MCK, Schéele C, Pedersen BK (2020) Exercise and browning of white adipose tissue – a translational perspective. Curr Opin Pharmacol 52:18–24
Shang H, Liu X, Guo H (2017) Knockdown of Fstl1 attenuates hepatic stellate cell activation through the TGF-β1/Smad3 signaling pathway. Mol Med Rep 16:7119–7123
Simon L, Jolley SE, Molina PE (2017) Alcoholic myopathy: pathophysiologic mechanisms and clinical implications. Alcohol Res 38:207–217
Singh SS, Kumar A, Welch N, Sekar J, Mishra S, Bellar A, Gangadhariah M, Attaway A, Al Khafaji H, Wu X, Pathak V, Agrawal V, McMullen MR, Hornberger TA, Nagy LE, Davuluri G, Dasarathy S (2021) Multiomics-identified intervention to restore ethanol-induced dysregulated proteostasis and secondary sarcopenia in alcoholic liver disease. Cell Physiol Biochem 55:91–116
Sobrino P, Ojeda ML, Nogales F, Murillo ML, Carreras O (2019) Binge drinking affects kidney function, osmotic balance, aldosterone levels, and arterial pressure in adolescent rats: the potential hypotensive effect of selenium mediated by improvements in oxidative balance. Hypertens Res 42:1495–1506
Spear L (2000) Modeling adolescent development and alcohol use in animals. Alcohol Res Health 24:115–123
Spear LP (2018) Author Correction: effects of adolescent alcohol consumption on the brain and behaviour. Nat Rev Neurosci 19:439
Sriram S, Subramanian S, Sathiakumar D, Venkatesh R, Salerno MS, Mcfarlane CD, Kambadur R, Sharma M (2011) Modulation of reactive oxygen species in skeletal muscle by myostatin is mediated through NF-κB. Aging Cell 10:931–948
Steiner JL, Lang CH (2015) Dysregulation of skeletal muscle protein metabolism by alcohol. Am J Physiol Endocrinol Metab 308:E699–E712
Steiner JL, Lang CH (2019) Ethanol acutely antagonizes the refeeding-induced increase in mTOR-dependent protein synthesis and decrease in autophagy in skeletal muscle. Mol Cell Biochem 456:41–51
Toyoda T, Hayashi T, Miyamoto L, Yonemitsu S, Nakano M, Tanaka S, Ebihara K, Masuzaki H, Hosoda K, Inoue G, Otaka A, Sato K, Fushiki T, Nakao K (2004) Possible involvement of the α1 isoform of 5′AMP-activated protein kinase in oxidative stress-stimulated glucose transport in skeletal muscle. Am J Physiol - Endocrinol Metab 287
Van Hall G, Steensberg A, Sacchetti M, Fischer C, Keller C, Schjerling P, Hiscock N, Møller K, Saltin B, Febbraio MA, Pedersen BK (2003) Interleukin-6 stimulates lipolysis and fat oxidation in humans. J Clin Endocrinol Metab 88:3005–3010
Funding
Funding for open access publishing: Universidad de Sevilla/CBUA This research was funded by the Andalusian Regional Government which supports the CTS-193 research group (2021/CTS-193; 2019/CTS-193) and VII Plan Propio de Investigación y Transferencia of University of Seville 2022. The first author has a predoctoral researcher and teaching personnel contract, number USE-22212-V, and also funded by the Andalusian Regional Government.
Author information
Authors and Affiliations
Contributions
Conception and design: M.L.O., J. D.C., and J. O.; development of methodology: F.N., M.L.O., M.D.C.G.L., I.R.H., and J.M.H.; analysis and interpretation of data (e.g., statistical analysis): O.C., J.D.C., and J. O.; writing—original draft preparation, M.L.O.; F.N., and I. R.H.; writing—review, M.L.O., M.D.C.G.-L., J. M.H., and O.C.; editing, F.N. and M.D.C. G.L.; visualization, M.L.O. and I.R.H.; supervision, M.L.O., J.D.C, J.O., and O.C.; management of reference, F.N. and J.M.-H; figures design, M.L.O. and F.N.; funding acquisition, O.C. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This manuscript does not contain clinical studies or patient data. The experimental protocol with Wistar rats was approved by the Ethics Committee of the University of Seville.
Consent for publication
All authors revised the manuscript and approved the version to be published.
Conflicts of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points:
1. BD during adolescence affects skeletal muscle oxidative, metabolic, and energy balance.
2. BD seriously alters myokine secretion, which has important endocrine repercussions.
3. BD via myokines promotes muscle atrophy and the insulin resistance process.
4. The altered myokine secretion also compromises hepatic and cardiovascular health.
Supplementary Information
ESM 1
(PDF 585 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Romero-Herrera, I., Nogales, F., Diaz-Castro, J. et al. Binge drinking leads to an oxidative and metabolic imbalance in skeletal muscle during adolescence in rats: endocrine repercussion. J Physiol Biochem 79, 799–810 (2023). https://doi.org/10.1007/s13105-023-00983-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-023-00983-z