Abstract
Introduction
Circulating endothelial cells (CEC) play an important role in tumor neovascularization and may have prognostic value in cancer patients. This study was designed to investigate the role of CEC as a marker for predicting platinum plus pemetrexed first-line chemotherapy efficacy in advanced non-squamous non-small cell lung cancer (NSCLC).
Methods
A prospective study was performed whose main objective was to study whether the numbers of CEC at baseline and prior to the second and third cycle of chemotherapy were response predictors. Sixty-nine patients received cisplatin plus pemetrexed, and peripheral blood samples were performed at baseline and after second and third cycle. Separation and CEC count were performed using inmunomagnetic separation (CellSearch).
Results
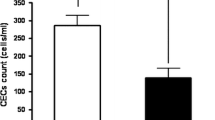
The CEC count in 4 mL of peripheral blood was obtained prior to the first, second, and third cycle of treatment. Baseline levels and evolution of CEC were correlated with response to treatment according to RECIST criteria after three cycles of treatment. Sixty-nine patients were included: 43 (64.2 %) received cisplatin/pemetrexed and 24 (35.8 %) carboplatin/pemetrexed. Range of baseline CEC: 8–965 (mean of 153 cel/4 mL). The results after 3 cycles were: 25 partial responses (36.2 %), 17 cases of stabilization of disease (24.6 %), 16 of progressive disease (23.2 %) and 11 non-evaluables (16 %). No significant relationship between the baseline CEC count and response was found (p value = 0.831). Increase >50 % between the first and second cycle was correlated significantly with progression disease (p = 0.008). Patients who had a baseline CEC count greater than the mean (>153 cells/4 mL) showed longer progression-free survival and global survival without statistical significance.
Conclusions
In this homogeneous group of patients with NSCLC, there is no correlation between response to treatment and CEC baseline levels. The increase in CEC numbers after the first cycle could be a negative predictive factor.



Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Foreman D, et al. Global cancer statistics. CA Cancer J Clin. 2011;61:69.
Murray CL, López AD. Alternative projections of mortality and disability by cause 1990–2020: global burden of disease study. Lancet. 1997;349:1498–504.
Govindan R, Page N, Morgensztern D, Read W, Tiernay R, Vlahiotis A, et al. Changing epidemiology of smallcell lung cancer in the United States over the last 30 years: analysis of the surveillance, epidemiologic, and end results database. J Clin Oncol. 2006;24:4539–44.
Ries L, Eisner M, Kosary C, eds. Cancer statistics review, 1975–2002. Bethesda, MD: National Cancer Institute, 2005.
Aggarval C, Somaiah N, Simon GR. Biomarkers with predictive and prognostic function in non-small cell lung cancer: ready for prime time? J NCCN. 2010;8:822–32.
Shantsila E, Blann AD, Lip GY. Circulating endothelial cells: from bench to clinical practice. J Thromb Haemost. 2008;6:865–8.
Shantsila E, Lip GY. Circulating endothelial cell in health and disease: how do we best quantify them? J Thromb Haemost. 2008;6:1021–4.
Beerepoot LV, Mehra N, Vermaast JS, Zonnenberg BA, Gebbink MF, Voest EE. Increased levels of circulating endothelial cells are an indicator of progressive disease in cancer patients. Ann Oncol. 2004;15:139–45.
Mancuso P, Burlini A, Pruneri G, Goldhirsch A, Martinelli G, Bertolini F. Resting and activated endothelial cells are increased in peripheral blood cancer patients. Blood. 2001;97:3658–61.
Woywodt A, Blann AD, Kirsch T, Erdbruegger U, Banzet N, Haubitz M, et al. Isolation and enumeration of circulating endothelial cells by immunomagnetic isolation: proposal of a definition and a consensus protocol. J Thromb Haemost. 2006;4(3):671–7.
Mancuso P, Antoniotti P, Quarna J, Calleri A, Rabascio C, Tacchetti C, et al. Validation of a standardized method for enumerating circulating endothelial cells and progenitors: flow cytometry and molecular and ultrastructural analyses. Clin Cancer Res. 2009;15:267–73.
Ronzoni M, Manzoni M, Mariucci S, Loupakis F, Brugnatelli S, Bencardino K, et al. Circulating endothelial cells and endothelial progenitors as predictive markers of clinical response to bevacizumab-based first-line treatment in advanced colorectal cancer patients. Ann Oncol. 2010;21:2382–9.
Matsusaka S, Suenaga M, Mishima Y, Takagi K, Terui Y, Mizunuma M, et al. Circulating endothelial cells predict for response to bevacizumab-based chemotherapy in metastatic colorectal cancer. Cancer Chemother Pharmacol. 2011;68(3):763–8.
Kondo S, Ueno H, Hashimoto J, Morizane C, Koizumi F, Okusaka T, et al. Circulating endothelial cells and other angiogenesis factors in pancreatic carcinoma patients receiving gemcitabine chemotherapy. BMC Cancer. 2012;12:268.
Bidard FC, Mathiot C, Degeorges A, Etienne-Grimaldi MC, Delva R, Pivot X, et al. Clinical value of circulating endothelial cells and circulating tumor cells in metastatic breast cancer patients treated first line with bevacizumab and chemotherapy. Ann Oncol. 2010;21:1765–71.
Malka D, Boige V, Jacques N, Vimond N, Adenis A, Boucher E, et al. Clinical value of circulating endothelial cell levels in metastatic colorectal cancer patients treated with first-line chemotherapy and bevacizumab. Ann Oncol. 2012;23(4):919–27.
Kawaishi M, Fujiwara Y, Fukui T, Kato T, Yamada K, Ohe Y, et al. Circulating endothelial cell in non-small cell lung cancer patients treated with carboplatin and paclitaxel. J Thorac Oncol. 2009;4:208–13.
Roodhart JM, Langenberg MH, Joost S, Lolkema MP, Baars A, Giles RH, et al. Late release of circulating endothelial cells and endothelial progenitor cells after chemotherapy predicts response and survival in cancer patients. Neoplasia. 2010;12:87–94.
Furstenberger G, von Moos R, Lucas R, Thürlimann B, Senn HJ, Hamacher J, et al. Circulating endothelial cells and angiogenic serum factors during neoadjuvant chemotherapy of primary breast cancer. Br J Cancer. 2006;94:524–31.
Rowand JL, Martin G, Doyle GV, Miller MC, Pierce MS, Connelly MC, et al. Endothelial cells in peripheral blood of healthy subjects and patients with metastatic carcinomas. Cytometry A. 2007;71:105–13.
Shaked Y, Bertolini F, Man S, Rogers MS, Cervi D, Foutz T, et al. Genetic heterogeneity of the vasculogenic phenotype parallels angiogenesis: implications for cellular surrogate marker analysis of antiangiogenesis. Cancer Cell. 2005;7:101–11.
Chu TQ, Ding H, Garfield DH, Gu AQ, Pei J, Du WD, et al. Can determination of circulating endothelial cells and serum caspase-cleaved CK18 predict for response and survival in patients with advanced non-small-cell lung cancer receiving endostatin and paclitaxel-carboplatin chemotherapy? A retrospective study. J Thorac Oncol. 2012;7(12):1781–9.
Fleitas T, Martínez-Sales V, Vila V, Reganon E, Mesado D, Martín M, et al. Circulating endothelial cells and microparticles as prognostic markers in advanced non-small cell lung cancer. PLoS One. 2012;7(10):e47365.
Zhu-Jun L, Jing W, Xi-Yin W, Chen P, Wang LC, Lin L, et al. Predictive value of circulating endothelial cells for efficacy of chemotherapy with Rh-endostatin in non-small cell lung cancer. J Cancer Res Clin Oncol. 2012;138:927–37.
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47.
Pagano M, Gauvreau K. 2000. Principles of biostatistics. 2nd ed. Belmont, CA: Duxbury.
Sandler A, Gray R, Perry MC, Brahmer J, Schiller JH, Dowlati A, et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med. 2006;355:2542–50.
Baggstrom MQ, Stinchcombe TE, Fried DB, Poole C, Hensing TA, Socinski MA, et al. Third-generation chemotherapy agents in the treatment of advanced non-small cell lung cancer: a meta-analysis. J Thorac Oncol. 2007;2(9):845–53.
Azzori CG, Baker S Jr, Temin S, Pao W, Aliff T, Brahmer J, et al. American Society of Clinical Oncology Clinical Practice Guideline update on chemotherapy for stage IV non-small-cell lung cancer. J Clin Oncol. 2009;27(36):6251–66.
Paz-Ares L, de Marinis F, Dediu M, Thomas M, Pujol JL, Bidoli P, et al. Maintenance therapy with pemetrexed plus best supportive care versus placebo plus best supportive care after induction therapy with pemetrexed plus cisplatin for advanced non-squamous non-smallcell lung cancer (PARAMOUNT): a double-blind, phase 3, randomised controlled trial. Lancet Oncol. 2012;13:247–55.
Wang J, Lou P, Lesniewski R, Henkin J. Paclitaxel at ultra low concentrations inhibits angiogenesis without affecting cellular microtubule assembly. Anticancer Drugs. 2003;14:13–9.
Beaudry P, Force J, Naumov GN, Wang A, Baker CH, Ryan A, et al. Differential effects of vascular endothelial growth factor receptor-2 inhibitor ZD6474 on circulating endothelial progenitors and mature circulating endothelial cells: implications for use as a surrogate marker of antiangiogenic activity. Clin Cancer Res. 2005;11(9):3514–22.
Patterson TA, Lobenhofer EK, Fulmer-Smentek SB, Collins PJ, Chu TM, Bao W, et al. Performance comparison of one-color and two-color platforms within microarray Quality Control (MAQC) project. Nat Biotechnol. 2006;24(9):1140–50.
Li H, Raia V, Bertolini F, Price DK, Figg WD. Circulating endothelial cells as a therapeutic marker for thalidomide in combined therapy with chemotherapy drugs in a human prostate cancer model. BJU Int. 2008;101(7):884–8.
Shaked Y, Henke E, Roodhart JM, Mancuso P, Langenberg MH, Colleoni M, et al. Rapid chemotherapy-induced acute endothelial progenitor cell mobilization: implications for antiangiogenic drugs as chemosensitizing agents. Cancer Cell. 2008;14(3):263–73.
Wang L, Wei J, Qian X, Yin H, Zhao Y, Yu L, et al. ERCC1 and BRCA1 mRNA expression levels in metastatic malignant effusions is associated with chemosensitivity to cisplatin and/or docetaxel. BMC Cancer. 2008;8:97.
Strijbos MH, Gratama JW, Schmitz PI, Rao C, Onstenk W, Doyle GV, et al. Circulating endothelial cells, circulating tumour cells, tissue factor, endothelin-1 and overall survival in prostate cancer patients treated with docetaxel. Eur J Cancer. 2010;46(11):2027–35.
Stubbe J. Ribonucleotide reductases in the twenty-first Century. Proc Natl Acad Sci USA. 1998;95:2723–4.
Gruenwald V, Beutel G, Schuch-Jantsch S, Reuter C, Ivanyi P, Ganser A, et al. Circulating endothelial cells are an early predictor in renal cell carcinoma for tumor response to sunitinib. BMC Cancer. 2010;31(10):695.
Yu HK, Lee HJ, Choi HN, Ahn JH, Choi JY, Song HS, et al. Characterization of CD45−/CD31+/CD105+ circulating cells in the peripheral blood of patients with gynecologic malignancies. Clin Cancer Res. 2013;19(19):5340–50.
Acknowledgments
Funding for this study was provided by Eli Lilly and Company; Eli Lilly and Company as such had no role in data collection, analysis or evaluation. CRO Pivotal provided advice to properly handle and submit the paper. Kavita Gandhi has reviewed and edited the manuscript language.
Conflict of interest
None author has any actual or potential conflict of interest including any financial, personal or other relationships with other people or organizations that could inappropriately influence (bias) their work.
Ethical standard
Ethics committees have been informed regarding all of this study procedures. Patients were properly informed and signed an informed consent.
Author information
Authors and Affiliations
Corresponding author
Additional information
On behalf of Grup ďinvestigació i divulgació en Oncologia (GIDO).
Rights and permissions
About this article
Cite this article
Sánchez Hernández, A., José Juan, O., Vidal Martínez, J. et al. Quantification of circulating endothelial cells as a predictor of response to chemotherapy with platinum and pemetrexed in patients with advanced non-squamous non-small cell lung carcinoma. Clin Transl Oncol 17, 281–288 (2015). https://doi.org/10.1007/s12094-014-1223-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12094-014-1223-5